7.5: Embryonic Development of the Axial Skeleton
- Page ID
- 20210
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)Learning Objectives
- Discuss the two types of embryonic bone development within the skull
- Describe the development of the vertebral column and thoracic cage
The axial skeleton begins to form during early embryonic development. However, growth, remodeling, and ossification (bone formation) continue for several decades after birth before the adult skeleton is fully formed. Knowledge of the developmental processes that give rise to the skeleton is important for understanding the abnormalities that may arise in skeletal structures.
Development of the Skull
During the third week of embryonic development, a rod-like structure called the notochord develops dorsally along the length of the embryo. The tissue overlying the notochord enlarges and forms the neural tube, which will give rise to the brain and spinal cord. By the fourth week, mesoderm tissue located on either side of the notochord thickens and separates into a repeating series of block-like tissue structures, each of which is called a somite. As the somites enlarge, each one will split into several parts. The most medial of these parts is called a sclerotome. The sclerotomes consist of an embryonic tissue called mesenchyme, which will give rise to the fibrous connective tissues, cartilages, and bones of the body.
The bones of the skull arise from mesenchyme during embryonic development in two different ways. The first mechanism produces the bones that form the top and sides of the brain case. This involves the local accumulation of mesenchymal cells at the site of the future bone. These cells then differentiate directly into bone producing cells, which form the skull bones through the process of intramembranous ossification. As the brain case bones grow in the fetal skull, they remain separated from each other by large areas of dense connective tissue, each of which is called a fontanelle (Figure 7.33). The fontanelles are the soft spots on an infant’s head. They are important during birth because these areas allow the skull to change shape as it squeezes through the birth canal. After birth, the fontanelles allow for continued growth and expansion of the skull as the brain enlarges. The largest fontanelle is located on the anterior head, at the junction of the frontal and parietal bones. The fontanelles decrease in size and disappear by age 2. However, the skull bones remained separated from each other at the sutures, which contain dense fibrous connective tissue that unites the adjacent bones. The connective tissue of the sutures allows for continued growth of the skull bones as the brain enlarges during childhood growth.
The second mechanism for bone development in the skull produces the facial bones and floor of the brain case. This also begins with the localized accumulation of mesenchymal cells. However, these cells differentiate into cartilage cells, which produce a hyaline cartilage model of the future bone. As this cartilage model grows, it is gradually converted into bone through the process of endochondral ossification. This is a slow process and the cartilage is not completely converted to bone until the skull achieves its full adult size.
At birth, the brain case and orbits of the skull are disproportionally large compared to the bones of the jaws and lower face. This reflects the relative underdevelopment of the maxilla and mandible, which lack teeth, and the small sizes of the paranasal sinuses and nasal cavity. During early childhood, the mastoid process enlarges, the two halves of the mandible and frontal bone fuse together to form single bones, and the paranasal sinuses enlarge. The jaws also expand as the teeth begin to appear. These changes all contribute to the rapid growth and enlargement of the face during childhood.
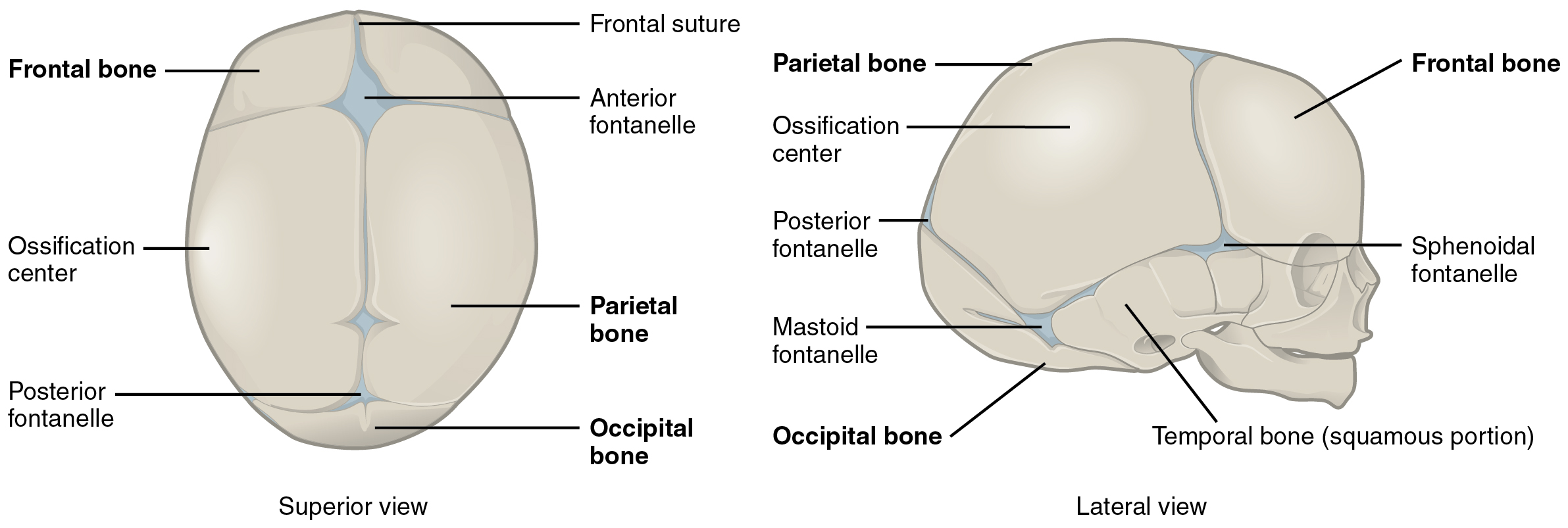
Figure 7.33 Newborn Skull The bones of the newborn skull are not fully ossified and are separated by large areas called fontanelles, which are filled with fibrous connective tissue. The fontanelles allow for continued growth of the skull after birth. At the time of birth, the facial bones are small and underdeveloped, and the mastoid process has not yet formed.
Development of the Vertebral Column and Thoracic cage
Development of the vertebrae begins with the accumulation of mesenchyme cells from each sclerotome around the notochord. These cells differentiate into a hyaline cartilage model for each vertebra, which then grow and eventually ossify into bone through the process of endochondral ossification. As the developing vertebrae grow, the notochord largely disappears. However, small areas of notochord tissue persist between the adjacent vertebrae and this contributes to the formation of each intervertebral disc.
The ribs and sternum also develop from mesenchyme. The ribs initially develop as part of the cartilage model for each vertebra, but in the thorax region, the rib portion separates from the vertebra by the eighth week. The cartilage model of the rib then ossifies, except for the anterior portion, which remains as the costal cartilage. The sternum initially forms as paired hyaline cartilage models on either side of the anterior midline, beginning during the fifth week of development. The cartilage models of the ribs become attached to the lateral sides of the developing sternum. Eventually, the two halves of the cartilaginous sternum fuse together along the midline and then ossify into bone. The manubrium and body of the sternum are converted into bone first, with the xiphoid process remaining as cartilage until late in life.
INTERACTIVE LINK
View this video to review the two processes that give rise to the bones of the skull and body. What are the two mechanisms by which the bones of the body are formed and which bones are formed by each mechanism?
HOMEOSTATIC IMBALANCES
Craniosynostosis
The premature closure (fusion) of a suture line is a condition called craniosynostosis. This error in the normal developmental process results in abnormal growth of the skull and deformity of the head. It is produced either by defects in the ossification process of the skull bones or failure of the brain to properly enlarge. Genetic factors are involved, but the underlying cause is unknown. It is a relatively common condition, occurring in approximately 1:2000 births, with males being more commonly affected. Primary craniosynostosis involves the early fusion of one cranial suture, whereas complex craniosynostosis results from the premature fusion of several sutures.
The early fusion of a suture in primary craniosynostosis prevents any additional enlargement of the cranial bones and skull along this line. Continued growth of the brain and skull is therefore diverted to other areas of the head, causing an abnormal enlargement of these regions. For example, the early disappearance of the anterior fontanelle and premature closure of the sagittal suture prevents growth across the top of the head. This is compensated by upward growth by the bones of the lateral skull, resulting in a long, narrow, wedge-shaped head. This condition, known as scaphocephaly, accounts for approximately 50 percent of craniosynostosis abnormalities. Although the skull is misshapen, the brain still has adequate room to grow and thus there is no accompanying abnormal neurological development.
In cases of complex craniosynostosis, several sutures close prematurely. The amount and degree of skull deformity is determined by the location and extent of the sutures involved. This results in more severe constraints on skull growth, which can alter or impede proper brain growth and development.
Cases of craniosynostosis are usually treated with surgery. A team of physicians will open the skull along the fused suture, which will then allow the skull bones to resume their growth in this area. In some cases, parts of the skull will be removed and replaced with an artificial plate. The earlier after birth that surgery is performed, the better the outcome. After treatment, most children continue to grow and develop normally and do not exhibit any neurological problems.

